-
November 15, 2021
Temperature Monitoring for Diabetic Foot Care is the Gold Standard
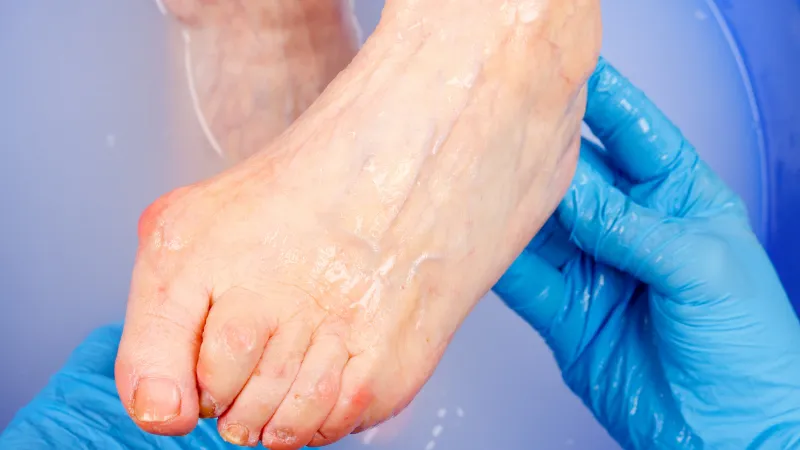

Remote patient monitoring (RPM) has brought to light a new preventative care option for people living with neuropathy and diabetic foot ulcers, both complications of diabetes. Without proper care, these conditions progress to deteriorating conditions like Charcot, or even worse, amputation of the affected limb.
Research shows that temperature monitoring in conjunction with regular visual exams can improve outcomes related to diabetic foot ulcers.(1) Temperature monitoring is the gold standard for diabetic foot care.
Preventing Diabetic Foot Ulcers with Remote Patient Monitoring (RPM)
Adopting strategies to prevent foot complications plays an increasingly important role in the management of patients with diabetes. The rapid expansion of remote patient monitoring opens the door for many physicians to introduce crucial limb-saving preventative care options.
“Preventing ulcers is very important in diabetic patients. Poorly healing ulcers, infected ulcers, and ulcers with poor circulation can lead to limb amputation,” says Dr. Puja Uppal, board-certified physician. “Many times ulcers may not hurt because the patient has loss of feeling due to neuropathy or vascular disease; thus, the patient might not be aware of a growing infection from an ulcer until it may be too late.”
“The prevention of ulcers in patients with diabetes is crucial because it prevents the onslaught of a host of other potentially serious health problems,” says Dr. Beverly Yates ND, an internationally acclaimed diabetes expert. “Ulcers in the feet of a diabetic can lead to gangrene and loss of the affected limb or infections that can become systemic (an infection that starts at the area of ulceration can spread from being local in the foot to the whole body, i.e. starting in a bone in the affected foot).”
In order to reduce costs and prevent poor patient outcomes, healthcare practitioners are quickly turning to Siren Socks’ remote temperature monitoring to help people with diabetes avoid foot ulcers and amputations.

Recognizing Inflammation Promptly
Inflammation is one of the first signs of an ulcer, which can be recognized early by identifying increased temperature to localized areas on the feet. Siren Socks are designed to improve patient outcomes related to diabetic foot ulcers and other diabetes complications.
This wearable device is embedded with micro-sensors that recognize temperature changes in the feet, offering rapid detection of inflammation and injury. Through Siren’s unique RPM platform, trained nurses can swiftly coordinate care with the patient’s doctor, improving the outcomes for many suffering from diabetic foot complications.
Patients wear their Siren Socks daily, which measure foot temperature at six locations to determine if inflammation occurs. When foot temperature goes up, this indicates early signs of inflammation and a licensed nurse calls the patient to check on any symptoms and maybe ask for photos. This is a crucial tool in ensuring patients with neuropathy receive guidance at the first signs of an ulcer—before it leads to more serious complications or amputation.
Clinical Results of Siren Socks
According to a study conducted by Dr. David G. Armstrong, professor of clinical surgery at Keck School of Medicine of USC, “skin temperature monitoring reduces the risk for diabetic foot ulceration in high-risk patients”.
This study looked at the data from 225 participants with diabetes who were at high risk for ulcerations. Each participant was assigned to one of two treatment groups, one of which used infrared temperature scans to check foot temperature. Over the course of this 18-month study, participants were monitored for a foot temperature difference greater than 4 degrees Fahrenheit. The results concluded that “High temperature gradients between feet may predict the onset of neuropathic ulceration and self-monitoring may reduce the risk of ulceration.” This clinical evidence sheds light on a new preventative approach that can substantially improve patient outcomes.
Temperature Monitoring: The New Gold Standard
Research demonstrates that temperature monitoring is a breakthrough diagnostic technology that can prevent ulcers from forming. The guidelines established by the International Working Group on the Diabetic Foot for foot ulcer prevention acknowledge that temperature monitoring can reduce and prevent the occurrence of ulcers in diabetic patients. Through prompt diagnosis and treatment, we can begin to take the necessary steps to prevent these ulcers from progressing into infection.
Managing diabetes and avoiding foot ulcers can be complex and requires daily care and maintenance from the patient. Remote patient monitoring with Siren Socks can help simplify the life of these patients while reducing the risk for diabetes-related infection that may lead to amputation. With remote patient monitoring (RPM), clinicians can track and treat diabetic foot ulcers at the onset — while relieving some of the burden to the patient. Through proper patient education and guidance, providers can improve patient compliance and create a more efficient system for the prevention and management of diabetic foot complications.
For some, RPM with Siren Socks can help ensure your diabetes and neuropathy are controlled. Siren Socks track your foot temperature and recognize inflammation at the onset. Trained nurses continuously monitor this data and coordinate care with your doctor when signs of inflammation or injury are detected. This reduces the risk of long-term injury associated with diabetes, peripheral neuropathy, and Charcot.
Interested in learning more about Siren Socks?
Siren Socks help patients and doctors find early signs of potential diabetic foot ulcers. Don’t take our word for it. Talk to your doctor about prescribing Siren Socks today!
[comment]
Related Blog Posts
Latest Articles
Siren Raises $9.5M, Led by an $8M Investment from Mölnlycke Health Care to Drive Diabetic Foot Ulcer Prevention and Management
Siren announces investment by Mölnlycke of $8 million to further development and adoption of Siren’s innovative diabetic foot ulcer prevention solution.
About Siren Socks
Siren Socks are smart socks that help detect potential issues with your feet. Siren Socks are an FDA-registered Class I medical device and are designed for people living with diabetes and neuropathy. The socks measure your foot temperature. Temperature monitoring has been shown to help reduce the number of diabetic foot ulcers in multiple clinical studies over the past 20 years and is considered the gold standard in diabetic foot care. The information from the socks is monitored by licensed nurses who contact you regularly to check on your health and the status of your feet. Your doctor reviews any issues that arise and determine if a clinic visit is necessary. Siren Socks are covered by Medicare, Medicare Advantage, and many private insurance plans. Interested patients can find a Certified Siren Provider near them and begin the enrollment process by clickinghere.